Rubella. part 1
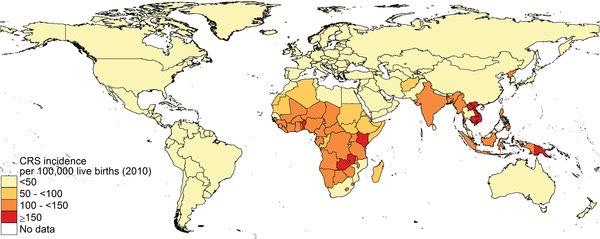
Rubella was considered eliminated from endemic transmission in the U.S. in 2004; sporadic cases reported since 2004 (under 10 annually in the U.S. since 2009) have been acquired during international travel to regions where rubella continues to be endemic, but outbreaks have not resulted from these introduced cases.
Practitioners in economically privileged societies are currently highly unlikely to encounter it. I bring it up here as it is a disease that is likely to return to the U.S., & therefore to the “developed” world at large, given the dismantling of federal public health safeguards, and as it has several interesting tales to tell.
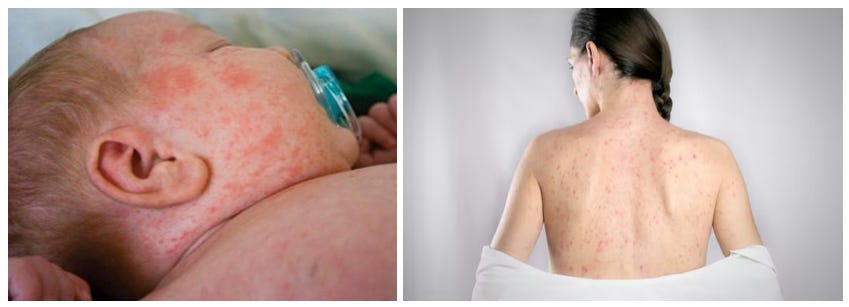
Rubella (“German measles,” “three-day measles”) is a typically mild disease. 25-50% of infections are asymptomatic; children may experience low-grade fever and a measles-like rash lasting 2-3 days following a prodrome of mild upper respiratory symptoms. Complications are rare; adult women may develop arthralgia. Pneumonia occurs rarely. 0.02% of cases may result in acute encephalitis.
The principal concern is Congenital Rubella Syndrome, involving transplacental transmission of the Rubella virus from a pregnant woman to her fetus, primarily during the first trimester (up to 12-16 weeks gestation), which may result in cardiac (patent ductus arteriosus, pulmonary valvular or pulmonary artery stenosis, or ventricular septal defect), cerebral, ophthalmic (congenital cataracts), and auditory (congenital deafness) birth defects, miscarriage or stillbirth, prematurity, low birth weight, neonatal thrombocytopenia, anemia, hepatitis, neonatal encephalitis, and neurodevelopmental disorders, including autism and rarely progressive rubella panencephalitis, similar to the subacute sclerosing panencephalitis of Measles. The risk of major defects in organogenesis is highest for infection in the first trimester. 80–90% of mothers who contract Rubella within the first trimester have either a miscarriage or stillbirth. This is a truly terrible disease, resulting in severe lifelong disability in those who survive. I saw a few cases in my training in the late 1970s, and hope to never see it again. The historically reported incidence of congenital Rubella is likely underestimated, as many cases likely terminated in first trimester miscarriage that may not have been reported or were not investigated as to cause. The seriousness of this typically mild and apparently inconsequential disease in the community may go unrecognized until cases of Congenital Rubella Syndrome appear.
Australian ophthalmologist Sir Norman Gregg first described what he termed Rubella Embryopathy following a Rubella epidemic in 1940, noting congenital cataracts of a unique nature often accompanied by congenital heart disease in children born to mothers who had experienced Rubella in early pregnancy.
Rubella was described by Daniel Sennert in 1619 and by Friedrich Hoffmann in 1740, who referred to it as Rötheln (Rötlich = “reddish” or “pink” in German), and was recognized as a disease distinct from measles and scarlet fever by George de Maton in 1814. As it was initially described by German physicians, it came to be known as “German Measles.” The British Royal Artillery surgeon Henry Veale described an outbreak in India in 1866, and coined the name “Rubella” (Latin “little red”). In the description of eruptive fevers, it became known as “third disease,” after Measles (Rubeola, “first disease”) and Scarlet fever/Scarlatina (“second disease”).
Congenital Rubella Syndrome, like paralytic Polio, might be considered a disease of the transition to modernity. Historically, it was likely that essentially all individuals were infected in early childhood, with typically mild, inconsequential disease and subsequent nearly lifelong immunity, periodically “boosted” by asymptomatic re-exposure, with only rare infections later in life. The improvements in general living conditions that reduced the incidence & mortality of other childhood diseases in the early 20th century reduced the incidence of rubella in early childhood, leaving young adults of childbearing age more frequently susceptible to infection
European colonial expansion into regions unaffected by endemic Rubella likely resulted in infection of adults of childbearing age; Congenital Rubella Syndrome was among the diseases that devastated the Indigenous peoples of the Americas and Oceana, and likely other regions of European colonial conquest, in the 15th-19th centuries.
A global Rubella pandemic in 1962-1965 started in Europe and spread to the U.S., resulting in the U.S. in 12.5 million cases, with 2,000 cases of encephalitis, 2,100 neonatal deaths, 20,000 infants born with congenital rubella syndrome, and 11,250 therapeutic or spontaneous abortions. Hospitals were overwhelmed, with entire units dedicated to caring for infants born with severe heart, hearing, and vision defects.
Rubella was made a reportable disease in the U.S. in 1966, and a formal surveillance program was established by the CDC in 1969.
(More to follow)